Epidemiologic studies consistently show that physical activity after diagnosis supports better breast cancer outcomes, and some research also indicates that women who increase their physical activity AFTER menopause may have a lower risk of breast cancer than those who do not.
Admit it.
You really, really want a secret weapon to wield far and wide; a weapon that empowers you with its pure strength and force, paving the way as you travel your breast cancer experience.
A secret weapon that potentially reduces risk, slays side effects, and manages to tame your tilted psyche.
We ALL want that.
And lucky you, that secret weapon is at your fingertips, only you may not know what it is, nor that it’s actually a weapon beholding of such power.
I’ll end your suspense.
That secret weapon is FITNESS.
Over the next six weeks I’m going to introduce you to the power of pure, raw physical fitness as an aid in doing all the things I mentioned above, plus, give you tips, strategies and Facebook LIVE videos to inspire and educate you on why it’s vitally important that you get moving and keep moving.
This week? I’m laying the foundation for what’s to come.

WHAT’S THE GOAL?
The goal of this 6-week series is not to convince you that you SHOULD exercise, only you can do that, but to encourage you to make fitness NON-NEGOTIABLE.
Anything in your life protected by a NON-NEGOTIABLE boundary is rendered sacred, free from the interference of outside circumstances, and becomes a priority at all costs.
That’s the level of reverence and importance to which I challenge you to raise your commitment to exercise.
Before I get started, let me be clear.
This series isn’t about exercise addiction, compulsion, or self-punishment; exercise behaviors of that sort are neither sacred, healthy, nor advocated by any credible fitness professional. If you find yourself heading down that path, I encourage you to seek help from a psychotherapist specializing in exercise addiction.
Why This Series?
Fitness is often written about and spoken to in the breast cancer world, but in more of a general way such as, “Exercise can reduce your risk of breast diagnosis or recurrence.”
While that’s a solid reminder, there’s so much more, like the why and how.
INTRODUCTION
It’s important to note that much of the evidence linking cancer risk to physical activity comes from observational studies – studies where individuals are observed or certain outcomes are measured. In the observational studies I reference, individuals report their physical activity and are followed by researchers who track the number and type of cancer diagnoses.
The data from this type of study gives us clues about the relationship between cancer risk and physical activity, but doesn’t definitively establish cause, as in “You won’t get cancer if you DO exercise, and you will get cancer if you DON’T.”
While we don’t yet have specific “do this, not that” data, my suggestion is to not wait for the specifics, but go with what we know. We know exercise is beneficial, and we have established guidelines for frequency, type and intensity. That’s not to say that those guidelines won’t change, but for now, they provide a solid road map we can follow.

Why Move?
A number of studies point to a lower risk of breast cancer (initial diagnosis and recurrence), typically a 20-30% reduction, in both premenopausal and postmenopausal women who are physically active, although there appears to be a stronger association for postmenopausal breast cancer.
Epidemiologic studies consistently show that physical activity after diagnosis supports better breast cancer outcomes, and some research also indicates that women who increase their physical activity AFTER menopause may have a lower risk of breast cancer than those who do not.
The menopausal timeline also plays a role in treatment approaches, for example, whether hormone-positive breast cancer is treated using tamoxifen or an aromatase inhibitor, so it makes sense that there may be a difference pre-and postmenopause for the fitness piece as well.
Research also suggests that more activity = lower risk. For example, engaging in your activity of choice for a longer period of time at a higher level of intensity appears to reduce risk more so than a shorter, more leisurely workout. One study in particular pointed to 30-60 minutes per day of moderate to vigorous activity being necessary to decrease risk, underscoring that there may very well be a dose-response relationship.

Why Now?
When you’re first diagnosed you have no physical impediments to exercise. You’re not experiencing medication, treatment or surgical side effects, and your energy level and physical ability isn’t compromised.
It may seem ludicrous to start a fitness program at the time of your diagnosis, when so much else demands your time and attention, yet research (and anecdotal reports) tells us that fitter bodies are better able to withstand treatment and recovery.
Between diagnosis and the start of treatment (surgery is considered treatment) there’s likely not enough time to see huge changes in your fitness level, but using fitness as a way to manage depression, fear, anxiety and anger is cathartic and lays the groundwork for doing any activity you can tolerate as you move along the continuum of treatment. (1)
If you’ve been sedentary and want to start now to engage in physical activity, it’s wise to request your doctor’s input. With everyone at different fitness levels and milestones in treatment, one-size-fits-all fitness recommendations don’t necessarily apply, so get clearance, listen to your own body, and do whatever you can tolerate.
HOW DOES IT WORK?
Exercise has a biologic effect on the body, which means at the cellular level changes take place that support risk reduction and improvement in your strength and/or stamina. (2)
- Levels of insulin, estrogen, and certain growth factors associated with breast cancer development and progression are reduced through physical activity.
- Surprisingly, exercise is not a panacea for weight loss, yet it can serve to help prevent and reduce obesity. Obesity is closely linked to insulin-resistance, a condition where the body’s cells fail to respond to insulin, leading to high blood sugar levels. Elevated levels of circulating blood sugar (vs. dietary sugar itself) are linked to increased breast cancer risk.
- Reduces inflammation, a condition that some research suggests may increase the risk of breast cancer recurrence.
- Improves immune system function, potentially by improving circulation, which allows the cells and substances of the immune system to move through the body freely to do their jobs efficiently.
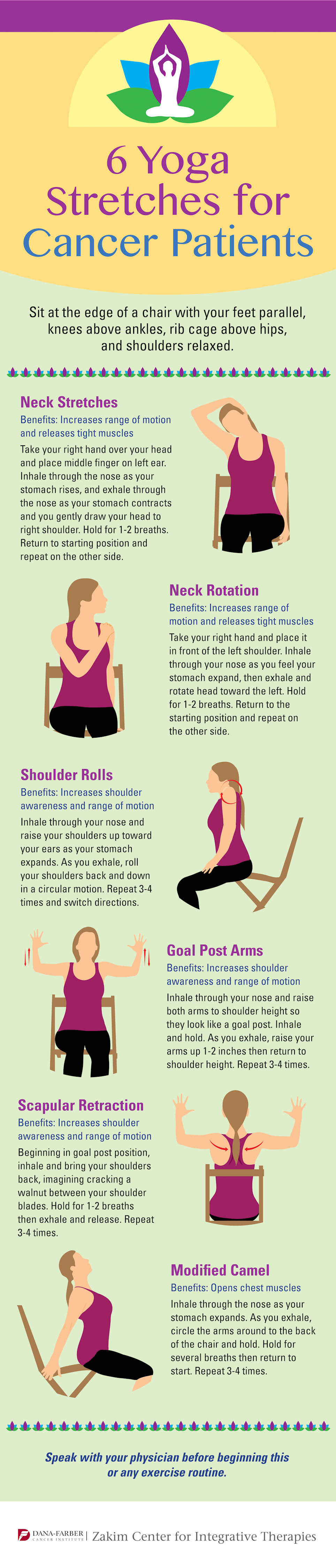
In the event that you just need a little something to get the blood flowing, here’s a collection of yoga stretches to try.
When you’re newly diagnosed, it’s normal to feel overwhelmed with trying to choose the best foods to eat, those to avoid, and how to make your new diet habits work in real life. To learn realistic tips and reliable education on how to best nourish your body, especially if you don’t know where to start, get help from me, a nutrition professional and breast cancer survivor. . .CLICK HERE.
Get your FREE Gear Up For Treatment Nutrition & Fitness Guide HERE!
SOURCES

